Treating gum disease can improve inflammatory diseases and boost longevity
Gum disease is shown to directly correlate with a series of systemic inflammation led diseases – from diabetes to rheumatoid arthritis - and with morbidity and mortality among humans, so more interdisciplinary collaboration between dentists and other medical professions is strongly called upon. Modern dentistry developed about a century ago and it evolved in line with human lifespan and longevity. Old and new studies about oral health and especially dental infections and gum disease are helping scientists connect the dots between oral health and longevity.
DENTAL RESEARCHSYSTEMIC HEALTHDENTAL INNOVATIONHEALTHCARE ETHICSLONGEVITY
Irene Petre
2/23/202611 min read


What is periodontitis?
Periodontitis is caused by infection in the gums and is a leading cause of tooth loss, bad breath and other wider health problems, including reduced life span and death. Circa 50% of adults in the UK have irreversible periodontal disease in some (1) form and about 40% of U.S. adults aged 30+ have some level of gum disease.
The disease isn’t only caused by food and poor brushing, but also by genetics (some people have more of a predisposition than others) and environmental factors (smoking, drinking, socio-economic status, levels of stress, medications and the presence of other systemic diseases such as diabetes or Alzheimer). It also correlates with age, which reinforces its link to Alzheimer, another age-related disease.
There is in fact a strong link between periodontitis and our immune system – when we say that stress and bad sleep hygiene are risk factors, we mean that they impact the immune system which can then produce distorted inflammatory responses in the body, including inflammation caused by bacterial infection in the mouth.
Sleep deficiency impairs the immune system's ability to combat oral bacteria and to heal gum tissue. Also research has shown that sleep deficiency sensitizes trigeminal TRPV1 neurons that innervate the gum tissue (periodontium). These neurons release substance P, a molecule that causes increased vascular dilation, permeability, and blood flow, leading to increased infiltration of inflammatory cells (neutrophils and macrophages) into the gums. Finally, elevated inflammation results in a higher expression of enzymes that destroy periodontal tissue and contribute to alveolar bone loss (2, 3).
Repeated or chronic sleep loss is associated with measurable increases in systemic inflammatory markers (notably IL‑6 and CRP) and can dysregulate immune signalling; a single night of total sleep loss usually has little effect, but several nights of partial sleep restriction do raise inflammation (4).
The link between periodontitis and other – mostly inflammatory - diseases reinforces the importance of integrated medicine and collaboration between various medical professionals and dentists
Apart from an important aesthetic aspect, good gums and oral health are indeed important for overall health and there is strong evidence showing a link between oral infections and periodontitis and other inflammatory disorders (such as rheumatoid arthritis, psoriatic arthritis, lupus) but also cardio-vascular diseases, diabetes, heart and lung diseases (such as pneumonia or chronic obstructive pulmonary disease or COPD), a series of cancers (colon, kidney, blood or pancreatic cancers) and neuro-degenerative diseases such as Alzheimer and Parkinson.
Studies have shown that periodontal disease may increase the risk of or exacerbate heart disease and overall cardio-vascular problems (11, 12). For example clinical research from the University College London in 2022 (13) shows that treating periodontitis slows the thickening of the inner two layers of the carotid arteries - the thickness of those artery walls is a key marker for cardiovascular disease risk (14).
Also patients at risk for infective endocarditis may require antibiotics prior to dental procedures (15) according to guidelines from major medical bodies such as American Heart Association (16) and European Society of Cardiology (16) - just one example why dentists, periodontologists and other medical specialists should work more closely together.
But bacteria associated with periodontal disease can be aspirated into the lungs and contribute to respiratory diseases as well, such as pneumonia – therefore improved oral care reduces pneumonia risk in high‑risk groups (17, 18, 19). Several reviews of older adults in hospitals and community settings show that improving oral care and gum disease reduces the risk of morbidity and mortality from aspiration pneumonia by as much as 67% (20, 21).
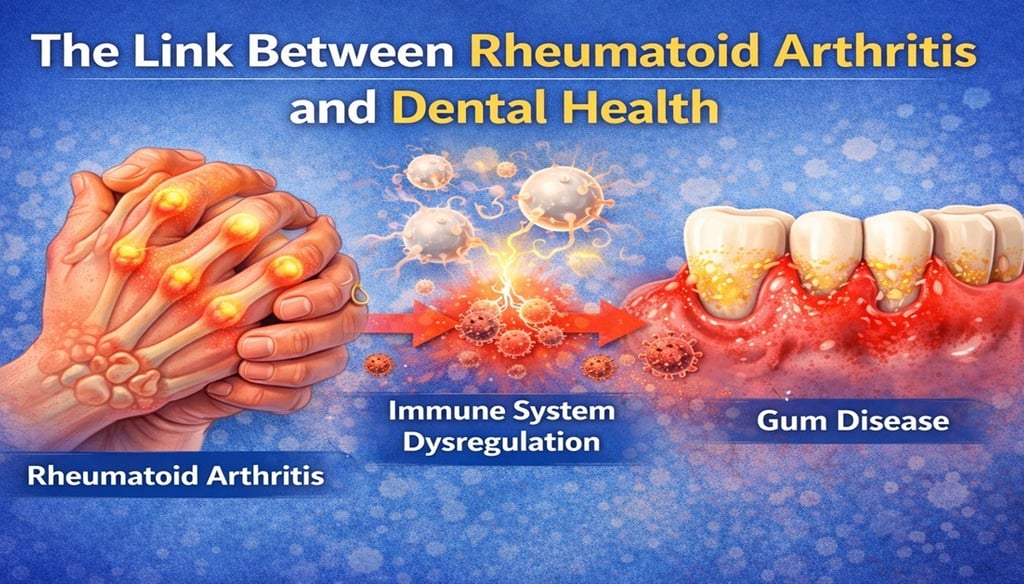
More recently a bi-directional link between periodontitis and auto-immune diseases like rheumatoid arthritis (RA) has been proven to exist - on February 12 researchers from the University of Birmingham have validated a two-way relationship between rheumatoid arthritis (RA) and periodontitis (gum disease), showing that treating gum disease can significantly reduce inflammation and improve RA symptoms for patients (22).
The study had 159 participants and investigated how microbial imbalances in the mouth (dysbiosis) contribute to systemic inflammation in RA patients. It showed that certain bacteria, such as Cryptobacterium curtum and Prevotella species, were strongly associated with RA and correlated with pro-inflammatory cytokines and that RA patients had higher levels of antibodies against oral pathogens, particularly Porphyromonas gingivalis, a bacterium linked to protein citrullination – a process involved in RA autoimmunity (22).
What is interesting is that severity of periodontitis strongly correlates with RA activity scores, including joint swelling and pain in this study. Intensive periodontal therapy (comprehensive non-surgical treatment approach designed to treat severe periodontitis by rapidly eliminating subgingival bacteria and inflammation) has been shown to improve RA symptoms and reduce antibodies against oral pathogens, re-setting a balance interaction between the immune system and oral microbes within 3 months according to the study.
The same researchers developed a rapid test for gum disease (a probe for use in point of care settings such as dental surgeries and pharmacies) that is meant to play a key role in early detection and monitoring of related heart and lung disease, type 2 diabetes and rheumatoid arthritis (23). It was initially developed to test for pre-diabetes and diabetes type 2, which represent an increasing problem in the UK. A main benefit the various researchers and medical professionals had in mind was "to explore the patient journey and identify barriers or challenges in the care pathway from oral health professional to general medical practitioner (GP) and back to the dental team” (24).
Unsurprisingly research can advance faster and new diagnostics and treatments be developed more effectively when dental and other medical specialists work closely together. Working together isn't often the norm since historically, medicine and dentistry are two separate education pathways and even within dentistry, dentists, lab technicians and periodontists follow very different study programs.
Evolution of the tooth-brush
From Egyptian times (left) to the first modern toothbrush with sterile nylon bristles (center) and up to the modern electric toothbrush of today (right)
An how about the link to longevity?
An increase in our average lifespan in the last hundred years is also due to improved oral care. Today the leading causes of death globally are heart and cardiovascular (CVD) diseases and cancer, whereas in 1920 - and previously in human history - infectious diseases (pneumonia/influenza, tuberculosis, diarrhoeal diseases or plague in previous centuries) were the main causes of death.
Improved oral care over the last century or so helped lower chronic oral infections, preserving teeth (and therefore chewing abilities for eating solid, nutrient rich foods) and reducing systemic inflammation (such as aspiration pneumonia). Together with vaccines and other advanced medical treatments, advanced dental and periodontal science has contributed to improved lifespan and longevity. In fact dental practice and life expectancy have developed in tack over the last 100 years: in 1910-20s the modern dental science started developing, in a period when average life expectancy in Europe was circa 50 years. Around 2023 (when dental practice started making another leap forward with an explosion of digital and AI solutions and new scientific studies being published), average lifespan in Europe was 81,4 years (25).
However, these benefits are not evenly distributed globally – in many parts of the world older people suffer from severe dental problems and gum disease. In fact the incidence of periodontal disease is highest in east sub-Saharan Africa (51%) and lowest in Oceania (10%) (26) and approximately 30% of world’s adults aged 65–74 years suffer from edentulism, where periodontal disease is the primary cause (27) – and this has a profound effect on the quality of life, aging process and morbidity and mortality rates.
In fact in 2016, the World Dental Federation adapted its definition of oral health from a previous narrow focus that included only disease, to a broader, multidimensional view that includes healthy aging and effectively “the ability to speak, smile, smell, taste, touch, chew, swallow, and convey a range of emotions through facial expressions with confidence and without pain or discomfort “ (28).
As shown good oral care reduces the risk of morbidity and mortality from aspiration pneumonia by as much as 67% (20, 21) and there are already proven bi-directional links between periodontitis and diabetes (the risk of developing diabetes is raised even in the presence of moderate periodontitis) and between periodontitis and RA and probably soon to be proven between it and Alzheimer (29).
Therefore there is strong evidence supporting the independent associations between periodontitis and common chronic inflammatory diseases of ageing, physical and emotional pain, mental health, confidence and optimism and overall quality of life.
Some sources
(2) https://www.pnas.org/doi/10.1073/pnas.2424169122
(5) https://perfectsmilespa.com/ancient-egyptian-toothpaste-a-5000-year-old-smile-secret/
(6) https://sci-hub.st/10.1038/sj.bdj.2009.309
(7) https://smj.org.sa/content/36/5/530
(8) https://www.deltadentalar.com/resources/blog/delta-dental/2019/03/13/history-of-toothpaste
(14) https://www.ahajournals.org/doi/10.1161/CIRCULATIONAHA.120.046361
(15) https://www.perio.org/for-patients/gum-disease-information/gum-disease-and-other-diseases/
(17) https://www.perio.org/for-patients/gum-disease-information/gum-disease-and-other-diseases/
(18) https://link.springer.com/article/10.1007/s40136-023-00455-4;
(19) https://www.mdpi.com/2227-9059/13/7/1741
(20) https://pubmed.ncbi.nlm.nih.gov/28387268/
(21) https://pubmed.ncbi.nlm.nih.gov/22390255/
(23) https://www.dentistrytoday.com/new-device-for-early-detection-of-gum-disease/
(26) https://www.thelancet.com/journals/lanhl/article/PIIS2666-7568%2821%2900142-2/fulltext
(27) https://www.who.int/whr/2006/whr06_en.pdf
(28) https://pubmed.ncbi.nlm.nih.gov/27885673/
(29) https://www.mdpi.com/2076-3417/15/12/6728
(34) https://www.bbc.com/news/articles/cj0nmj72v8ro
(36) https://brentmaxsondmd.com/blog/can-teeth-whitening-damage-gums/#:~:text=Conclusion,FAQs
(39) https://www.grandviewresearch.com/horizon/outlook/cosmetic-dentistry-market/europe
Note:
Infection is the invasion and multiplication of disease‑causing microbes (bacteria, viruses, fungi, parasites); inflammation is the body’s protective immune response to injury or harmful stimuli (which may include infection).
Infection can cause inflammation, but inflammation also occurs without infection (for example in autoimmune disease or physical injury).


For most of our history, people lacked proper products and technology for oral care
Old Egyptians used abrasive tooth powders mixed with resins and aromatic gums such as myrrh as antiseptic pastes and mouth rinses and miswak plant to treat gum disease and dental inflammation (5, 6). Ancient populations in the Middle East also used miswak from the Salvadora persica plant as a chewing stick and topical agent – and there is recent clinical and laboratory evidence that miswak has antibacterial, antiplaque, anti‑inflammatory, and anti‑halitosis properties and can help reduce gingival bleeding and plaque (7). These powders however lacked the potency of today’s compounds and our ancestors – from antiquity to the 19th century lacked basic tools for oral care, therefore tooth loss was very common among all past civilisations and social classes.
Whilst Egyptians are thought to be the first ones to have invented some sort of toothpaste (it was effectively an abrasive solution containing crushed eggshells, pumice, ox hooves' ashes and myrrh) around 5000-6000 years ago (8), modern toothpaste was only born in 1914 when fluoride was added to a previous cleaning paste, to help prevent decay and whitening agents to brighten teeth were only introduced in the mid 1980s (8). The modern sterile toothbrush using nylon bristles wasn’t made until 1938 (9) - previously people used horsehairs, feathers or pigs' hair for the bristles - none of which were very clean or sterile (9).
Ancient populations didn’t have the technology to properly care for their gums and teeth, let alone effectively treat them (whilst prehistoric dental drilling, extraction and fillings go back 14,000 years (10) - they remained painful, imprecise and subject to infections for most of our history), but today we have a vast array of professional dental treatments and off the counter solutions and there is enough evidence to indicate that an increase in our average lifespan in modern times is also due to improved oral care.






In the quest for longevity and personal enhancement though cosmetic dentistry, we need not forget the ethics
As more media and healthcare specialists are talking about longevity, AI and science, more and more people seem to develop some form of "medical and dental FOMO" (Fear of Missing Out on new medical treatments) or some form of digital health anxiety, especially among younger adults, experiencing anxiety about missing out on health trends, wellness or bio-hacking to preserve their youth - one such trends is cryotherapy, increasingly popular with GenZ in the UK (31); another one is of course cosmetic dental treatments (32) . This is not only affecting the young, but since the pandemic the older generations have started paying increasing attention to medical news (33) and new gadgets (such as smart watches monitoring various health parameters, nootropics, various brain and muscle stimulating and of course dental solutions).
As fitness and bio-hacking are becoming more extreme (from Hyrox (34) to cryotherapy), so are cosmetic dental treatments, in line with the times. Cosmetic dentistry is experiencing a significant surge in demand, driven by the "influencer-effect" of social media and tech advances with more extreme transformations being sought out (35), that often are purely cosmetical and can sometimes negatively affect the gums.
Some of these extreme treatments include:
ultra-thin and no-prep veneers, sold off the counter and which still involves permanent alteration of the enamel and potential infections and gum disease
instant laser whitening - while whitening is common, the demand for 8–10 shades lighter in a single, 1-hour session is increasing; this is more teeth bleaching and can not only damage the enamel but also the gums (36)
laser gum contouring - laser is used to precisely remove and sculpt excess gum tissue to expose more of the tooth, enhancing tooth-to-gum proportion; but removing too much tissue can lead to complications like gum recession and exposed roots, which may make teeth more vulnerable to future caries or sensitivity
comprehensive "full smile makeovers" - complete, full-mouth transformations, A combination of veneers, crowns, gum reshaping, and whitening to achieve the perfect smile (37).
Technological costs and pressure on reimbursement for standard procedures are becoming more important problems for dentists, so the temptation to focus on dental cosmetic procedures is also on the rise - in the UK (38) but also in other countries in Europe, with an expected annual growth rate of c. 12% between 2023 and 2030 (39). Cosmetic dental treatments are very expensive and often not covered by national healthcare systems or insurance policies. As demand for these costly procedures is surging - affordability for vital dental treatments is going down. Dental specialists should not forget about the importance of prevention and good access to necessary dental treatment and prioritise these aspects and genuine dental needs over cosmetic treatments, although they can look less lucrative in the short term.
But as with many other healthcare aspects, the role of policy makers in Europe remains key as through their policies they can shape access to periodontal care (through better public subsidies of essential periodontal services) and regulate cosmetic dentistry. Prevention first investment programs would do much in this sense as well as improving training and credential rules in this space and regulating advertising and medical devices and products.
IGEA Healthcare
Strategic Advisory for Life Sciences
Switzerland, UK, Italy
contact@igeahealthcare.com
© 2025 - 2026. All rights reserved.
